
Back pain is a common ailment that just about everybody in the U.S. has or will experience in their life at least once. In fact, more than 30 million people in the U.S. experience low-back pain at any point in time, according to the American Chiropractic Association. Some individuals have such debilitating back pain that they choose to have surgery. Unfortunately, back surgery isn’t always a success.
Failed back surgery syndrome (FBSS), just like back pain, can involve a tremendous amount of discomfort, and can result in long-standing chronic pain. However, you can find relief with medical marijuana for failed back surgery syndrome.
Failed back surgery syndrome refers to having persistent or new pain following surgery for leg or back pain. The term means you have a continuing pain condition and doesn’t necessarily imply there was a problem during surgery.
The pain can become worse within a couple of months after your surgery. It could be the result of built-up scar tissue around the spinal nerve roots, persistent muscle spasms and/or tissue pain.
Although reports are estimating a 20 to 40 percent incidence rate of FBSS as published in the Journal of Pain Research, the chances of developing it are much greater when you have repeated surgery. It’s also more prevalent in areas where spinal surgery is frequent.
Initially, it can be difficult to tell if you are experiencing FBSS symptoms or not since there will be some degree of discomfort and pain after traditional spine or back surgery during your recovery.
Just like each person’s symptoms won’t be the same before spine or back surgery, symptoms of FBSS will also vary between patients.
Some common symptoms of FBSS, however, include:
While FBSS doesn’t always develop following back or spine surgery, some factors can play a role in developing this condition, including:
Surgeons who don’t see many individuals with degenerative spine conditions are often less specialized and experienced in the diagnosis and treatment of these conditions. Because of this, when a relatively inexperienced surgeon tries to determine the underlying cause of the individual’s back or neck discomfort, they may try to correlate the pain pattern in the patient’s pain with a specific degeneration area in the spine.
Also, other sources of pain like hip osteoarthritis can cause similar symptoms and therefore the surgeon attributes them to a degenerative spine condition. They then perform the procedure at the wrong spine level or treat the condition improperly based on the improper diagnosis that leads to failed back surgery syndrome.
The body will form bands of scar tissue after any tissue disturbance as part of your body’s natural healing process. Spine or back surgery is a good example of tissue disturbance. The fibrous adhesions can bind a nerve root and lead to a condition known as epidural fibrosis that can then turn around and cause FBSS and postoperative pain.
If the treating surgeon makes a technical error like leaving behind some herniated disc material or bone fragment that’s pressing on the spinal cord or nerve root, it can lead to pain that persists or worsens after surgery.
The goal of a standard spinal fusion surgery is to remove a damaged disc and stabilize the adjoining vertebrae with implants or bone grafts that are fortified naturally as the body heals following a procedure, to relieve nerve compression.
But to address back or neck pain successfully through spinal fusion, the surgeon needs first correctly to identify the patient’s source of pain. Plus, each patient will heal at a different rate. Since part of the healing process is vertebral fusion, it could take several months for some patients to achieve a solid fusion, while in others it never fully occurs.
When the surgeon decompresses a nerve root through surgery, it usually causes inflammation temporarily, and until this inflammation goes away, it can result in increased pain. In rare cases, however, there can be nerve damage that leads to symptoms like weakness and chronic pain in certain groups of muscles.
In some cases, after the surgeon places an implant, it can shift. Usually, this happens during recovery before the healing process of your body has reached the point where the implant firmly attaches to the vertebrae.
When an implant moves out of the location it’s intended, it’s less effective or can be ineffective at stabilizing the spine. Also, if a shifted implant is compressing sensitive neural tissue, it can cause a new, painful spine condition.
FBSS can cause complications such as:
To get through the initial part of further treatment, you’ll need to plan some coping skills.
When you’re looking forward to a substantial improvement only to have a setback, it can be an emotionally difficult time for you to adapt to the different outcome. This may cause anxiety or a low mood and make it more difficult for you to cope with the pain.
Although the physical symptoms of FBSS prompted you to see the doctor after surgery and are most definitely frustrating, you also need to consider the emotional and mental toll FBSS can have on you. When conservative treatments fail and back surgery is your last resort, experiencing the same, or new, pain because of your back surgery can cause you to start feeling an immediate sense of hopelessness. One study shows patients with FBSS experience poor quality of life, worsened pain, anxiety and depression.
Statistics relating to FBSS show around five to 40 percent of individuals undergoing lower spinal surgery develop FBSS as a complication.
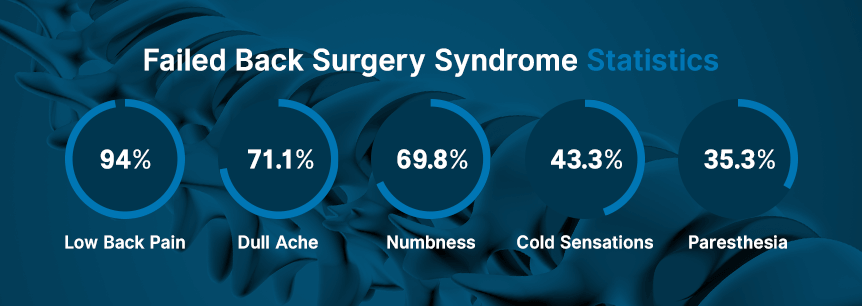
According to a 2017 survey, data regarding patient satisfaction and residual symptoms of 1,842 lumbar surgery patients showed a 20.6 percent FBSS prevalence rate, with other prevalence rates after surgery including:
Doctors have several treatment options if you have failed back surgery syndrome. These include the following.
The first line of treatment might involve nerve blocks, injections or a treatment to temporarily block radiofrequency neurotomy, or pain signals, that heats the affected small nerve endings.
Additionally, for these treatments for pain relief, the doctor may also recommend an exercise program during your recovery to recover muscle strength gradually.
If you’re experiencing disabling pain and don’t respond to these treatments, another option might be neuromodulation treatment:
It’s important doctors know and understand the spine thoroughly to make an accurate diagnosis and provide the right treatment. Future enhancements in diagnostic abilities with imaging modalities and new MRI might help doctors screen patients better with real physical pain generators as opposed to patients with more psychologically driven or non-physical pain.
There’s also new research on different recruitment patterns of core muscles in people with or without chronic back pain. This research has helped researchers understand why certain individuals often have recurrent bouts of back pain.
It can also help them find better therapy alternatives instead of surgery to treat individuals and potentially help avoid generating another generation of individuals at risk for FBSS following unsuccessful back surgery. To date, more than 50 clinical studies for failed back surgery syndrome have been completed, are in progress or are in the recruiting stage.
People have used cannabis for medicinal purposes since ancient times, and tens of thousands of modern alternative therapy doctors in various countries recommend the herb to their patients for pain control. Marijuana’s pain-relieving ability given in inhaled or oral forms has been underscored through many studies and stands up to rigorous evidence-based medication standards.
The cannabinoids in medical marijuana and failed back surgery syndrome treatment have been shown to act as a pain reliever in animal models in just about every experimental pain paradigm in spinal, peripheral and supraspinal regions involving both descending and ascending pain pathways. A 2012 review published in The Clinical Journal of Pain on cannabinergic pain compounds showed that 71 percent of the 38 published trials that met the criteria for inclusion demonstrated a positive analgesia outcome.
Not all cannabinoids in marijuana for failed back surgery syndrome produce a “high,” but they still provide a lot of therapeutic and medical value. Breeders can grow cannabis plants to have more amounts of nonpsychoactive cannabinoids that are still therapeutic. Cannabinol (CBN) and cannabidiol (CBD) are examples of these types of cannabinoids and can help modify the effects of the psychoactive cannabinoid THC. They also have therapeutic effects.
CBN, for instance, seems to act as a sedative and anticonvulsant. It also has other pharmacologic properties, like being able to induce sleep.

Due to medical marijuana assisting with inflammation and pain, doctors increasingly use cannabis as a treatment option for patients with back pain. Marijuana and failed back surgery syndrome treatment can help with symptoms such as:
Medical pot is growing in popularity as a preferred treatment for chronic back pain patients. While other conventional treatments can effectively treat back pain symptoms, they can also produce negative side effects like stomach upset, nausea, gastric bleeding and ulcers.
Medical cannabis can be an alternative medication for treating back pain and doesn’t have the same harsh side effects like those of the chronic pain medicines. Medical marijuana for failed back surgery syndrome can ease your back pain in the following ways:

Below are some potentially helpful strains when you struggle with FBSS:
For trouble sleeping, you need to pick the right strain, or it could have an opposite effect. Most indica strains aid with sleep, unlike sativas, which are more stimulating. Some good strains for sleep are:
To relieve anxiety, try these strains:
For depression, consider these strains:
When you’re just starting out with marijuana and failed back surgery syndrome treatment, you might not know which strains work best for your pain, but a cannabis doctor or staff member at a dispensary can help.
To find relief, use medical marijuana internally or topically. Some good methods are:
Smoking marijuana can have unwanted respiratory side effects, so consider other medical cannabis consumption methods. For instance, topicals in the form of creams applied directly to the pain site might be beneficial to relieve your discomfort.

To obtain more information on medical cannabis use to relieve your failed back pain symptoms, book an appointment with a marijuana doctor. Or, if you’re concerned about the negative side effects of conventional pain-relieving medicines are having on your health, Marijuana Doctors can help you improve the quality of your life. We have an abundance of resources for patients to help you learn more about medical cannabis and the many benefits it offers for a wide range of symptoms and conditions. Search for a dispensary or doctor with us today.
Find A Doctor Find A Dispensary


Please allow us to access your location to find local dispensaries.
VIEW ALL DISPENSARIES ➔