
Unfortunately, there’s no cure for herpes simplex virus. However, you can still treat the symptoms. Medical cannabis for herpes not only helps treat the symptoms, but it also can potentially prevent future viral outbreaks.
Marijuana for herpes is a useful alternative treatment option that just may help with the spreading of herpes. In this instance, not all cannabinoids are successful. However, THC has been shown to regulate T-lymphocyte functions and immune response to counter the viral infection.
THC mildly binds with cannabinoid receptors in the lymphoid cells and brain. The cannabinoid receptors in these tissues influence viral gene activation and immune signaling in response to THC dosage and binding. A study concluded THC interferes with DNA replication processes in a dose-dependent methodology, and therefore inhibits viral lytic replication — aka viral reproduction.
Another study conducted in 2010 tested a cannabinoid-filled facial lotion on individuals with postherpetic neuralgia, a pain disorder similar to shingles, and found the cream decreased the pain by 87 percent. Newer studies are suggesting various components in the marijuana plants might produce similar effects for the outbreaks of herpes.

CBD helps combat both the immune response and inflammation of HSV outbreaks. This cannabinoid is an anti-inflammatory, and dozens of scientific publications recognize it for its ability to fight off foreign pathogens like viruses and initiate tissue and cell repair.
There are some side effects of marijuana, including:
Find A Doctor Find A Dispensary
Medical marijuana for herpes helps with symptoms such as:
Medical weed can help sufferers of herpes in various ways. It can help reduce anxiety that surrounds big events and everyday life, which can trigger outbreaks. Each cannabinoid has differing effects, but CBD appears to be more effective at decreasing anxiety.
CBD, with its anti-inflammatory effects, can also help reduce the pain and severity an HSV outbreak causes.
THC can help decrease pain an outbreak causes. Individuals with herpes typically experience neuropathic pain, which medical pot is especially effective at targeting.
Whether you roll the herb into a joint, use edible forms or vape it, various strains of the plant can significantly decrease the discomfort of HSV.
Some good medical marijuana and herpes strains include:
It’s likely you’ll find both external and internal applications of cannabis for herpes to help your condition. By smoking cannabinoids or ingesting them orally, you’re already boosting your immune system. Marijuana has strong antiviral properties. There are even specific strains bred for this trait.
Along with this, you may want to consider topical treatment. THC creams and oils seem to stop both the pain and progression of the sores.
Even though a herpes outbreak isn’t constant, the sores are still painful and itchy — not to mention unattractive. CBD oil has been shown to alleviate this pain and itchiness, calming your cold sores and reducing their redness and pain. And, even though you can’t cure herpes, CBD oil does weaken the virus, so you have fewer outbreaks.
If you have a cannabis-friendly doctor, you should talk to them. They may be able to recommend certain strains you can get started with. You can also discuss this with your local dispensary, even if you wish to be discreet about your particular condition.
If you don’t have a cannabis-friendly doctor, you can find one here at Marijuana Doctors. We even have a long list of dispensaries to help you find one in your area. To learn more about using medical marijuana to relieve your symptoms of HSV, book an appointment through MarijuanaDoctors.com today.
Find A Doctor Find A Dispensary
Herpes simplex virus, also called HSV or herpes, is a viral infection that can affect different parts of your body. There are two types of HSV: HSV 1 and HSV 2.
HSV 1 causes cold sores around your face and mouth, while HSV 2, or genital herpes, affects your buttocks, genitals and anal area. Other herpes viral infections can affect your skin, eyes and other body parts. HSV can be harmful both in individuals with a weak immune system and in newborn babies. HSV is extremely contagious and easy to spread through direct contact, even when there are no visible sores.
Many individuals who get HSV never feel or see anything. When they do have symptoms, they may experience:
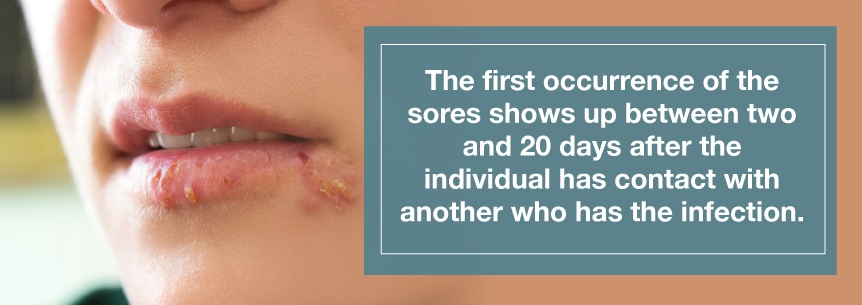
One or more fluid-filled, painful blisters will pop up. The blisters break open and usually ooze fluid, form a crust and then heal. The first occurrence of the sores shows up between two and 20 days after the individual has contact with another who has the infection. The sores may last anywhere from seven to 10 days.
Depending on the type of HSV, the blisters may appear on your:
Some individuals will get the sores near the spot on their body where the virus entered. Others won’t experience any symptoms. The lesions turn into blisters and become painful and itchy before they heal. When they do improve, they don’t go away entirely. The infection remains dormant inside your body, and can flare up anytime.
Your skin may itch, burn or tingle for a day or so before the blisters appear.
Individuals — usually women — with genital herpes might have a burning feeling when urinating or have trouble urinating.
You may experience flu-like symptoms such as muscle aches, fever or swollen lymph nodes in the groin or neck.
Sometimes the HSV can spread to one or both of your eyes. Medical professionals refer to this as herpes keratitis, representing an infection in your cornea. When this happens, you might experience:
If you leave this untreated, it can result in scarring of your cornea, which then can cause cloudy vision or even worse, vision loss or blindness.
If you develop symptoms of HSV, you could have these for as long as:
You can contract one of two main types of HSV:
However, this is not an absolute distinction. Genital herpes can also occur from HSV-1.
After the initial HSV infection, like other herpes viruses, HSV stays dormant or latent in your body for the rest of your life. An inactive infection might not cause symptoms again, or it could reactivate periodically. Triggers that reactivate HSV include emotional stress, menstruation, a fever, physical trauma, overexposure of your lips to sunlight or having a dental procedure. A suppressed immune system could also trigger reactivation. For instance, if you are taking anti-rejection medications for an organ transplant, you may experience a reactivation.
As mentioned, HSV is very contagious, and spreads through direct contact. Children will usually contract HSV-1 through early contact with an infected adult. Once they contract the viral infection, they carry it for the rest of their lives.
You can contract HSV-1 through general interactions like:
The virus can spread faster when an infected individual has an outbreak. Around 30 to 95 percent of adults are HSV-1 positive. However, they might never have a flare-up. You can also contract genital herpes from HSV-1 if you perform oral sex with a person who has cold sores at that time.

You can contract HSV-2 through different forms of sexual contact with an individual with HSV-2. According to the American Academy of Dermatology, approximately 20 percent of U.S. adults who are sexually active have the HSV-2 infection. Although you can spread the HSV-2 infection through a herpes sore contact, most individuals get HSV from people who don’t have any sores.
There could be complications with the HSV infection, including the following.
It’s not uncommon for individuals who receive a diagnosis of herpes to develop depression. Two common causes of depression following a diagnosis of herpes are shame and fear of infecting a partner.
A national study published in a 2012 edition of the journal Sexually Transmitted Infections found adults with the HSV-2 infection were twice as likely to develop depression as adults who didn’t have HSV-2.
Herpes might increase your depression. However, depression, anxiety and stress can cause an increase in an outbreak of herpes. Many studies have associated an uptick in depression and stress to more frequent outbreaks. That shouldn’t come as a surprise, as depression and stress can severely affect the immune system. That is one reason why you should seek help if you’re anxious or stressed after receiving a new herpes diagnosis.
Facts about HSV, according to the World Health Organization, include:
Researchers have found the evolutionary origins of human HSV-1 and HSV-2 and reported HSV-1 infected hominids 6 million years ago before their evolutionary split from chimpanzees. HSV-2 hopped from primeval chimps to Homo erectus — ancestors of modern humans — around 1.6 million years ago.

Treatments are available to ease your herpes simplex virus symptoms, even though there isn’t a cure. An antiviral ointment or cream can help relieve the itching, burning or tingling. Antiviral drugs, either pills or intravenous shots, can shorten a herpes outbreak.
Prescription antiviral medications approved for treating HSV are:
Side effects of antiviral medicines may include:
When you take these medications daily, they can lessen the frequency and severity of outbreaks. They can also help prevent infected individuals from spreading the viral infection.
You can relieve the pain linked with genital sores with a warm bath.
Many types of vaccine, both therapeutic and prophylactic, in the past decade, have contained a replication-defective HSV, glycoproteins or viral DNA. New research focused on immune evasion by the viral infection has involved the development of vaccines with numerous gene manipulations and deletions, combined with the use of more new specific adjuvants.
Additionally, new “prime-boost” techniques of strengthening the efficacy of vaccines have been promising, but there were also flaws in some recent methods that appear to have compromised the effectiveness of the vaccines in humans.
Also, more than 200 clinical trials have been or are in process to study the herpes simplex virus.


Please allow us to access your location to find local dispensaries.
VIEW ALL DISPENSARIES ➔